Two days before she was set to fly across the country to start her new life as a graduate student at Duke University School of Medicine last summer, Elena Roberts visited her primary care nurse practitioner. She needed some vaccination records and a signature.
Roberts, who graduated from The University of Portland’s College of Arts and Sciences last May, was excited about the opportunities ahead, but in the days before her flight to North Carolina, she was stressed, rushing around her hometown of Medford, Ore. trying to cross everything off her to-do list.
The next day, Roberts received a call from the doctor’s office — strange, since it was her provider’s day off.
Roberts obtained the signature she needed, but could not fly to North Carolina.
At her appointment, Roberts inquired about persistent lower back pain and a swollen lymph node in her neck, two nagging symptoms she did not expect to be related. Although her nurse practitioner did not suspect anything serious, she suggested that they do a CT scan “just to be safe.”
She was alone when she drove to the clinic that Wednesday after receiving the unexpected call. Of that meeting she recalls few but the words: “You have cancer.”
Roberts, who lost her mother at the age of 10 to heart disease, was raised by her grandmother and her godparents.
At the time of her diagnosis, her godparents were in meetings, her boyfriend in another state and her friends spread all over the country. So she sat with her nurse practitioner in the small room, and then alone for a while, and cried.
Having calmed down a little, Roberts knew she needed to tell her loved ones. When she rang her boyfriend, John O'Halloran, he was out to lunch with family in Houston, Texas.
Roberts shared the news in the careful, scientific manner of a pre-med student: She had Hodgkin's Lymphoma, specifically Nodular Sclerosing.
O’Halloran’s mind started reeling.
“Alright,” he told her, “It's just a bump in the road. We will get through it.”
But his measured voice was no reflection of what was going through his head. As someone whose family had been affected by cancer on multiple occasions, he couldn’t help but wonder, “Again? Really?” and, “ She’s so young. Why? Why now?"
He had not suspected that the symptoms she started experiencing less than a year earlier would have ever amounted to something so serious.
“But I never felt like I was going to die,” Roberts told The Beacon in a coffee shop six months later. “I was just scared that I was going to have to put my whole life on hold.”

Senior Year
Roberts, who graduated from UP with a degree in biology and a minor in neuroscience, first started experiencing symptoms during the summer before her senior year. Lower back pain that she initially attributed to her Ikea futon bed persisted long after she moved into Haggerty-Tyson to start her senior year. O’Halloran, also a UP alumnus (‘15), encouraged her to try a Tempurpedic mattress and she did, to no avail.
In September, when her pain started waking her up at night, she visited her primary care doctor. They wondered if it could be sciatica, a condition in which pressure is inflicted on the sciatic nerve and causes pain to the core and back, and offered her opioids for temporary pain management.
She laughs about that now. “I said no!”
She continued to experience regular lower back pain through the fall and winter, and when the pain moved into her abdomen, she wondered if the problem could be dietary. Like many 20-something Portlanders, Roberts was health-conscious.
She was losing weight, too, but credited BurnCycle and healthy eating.
In February, Roberts looked in the mirror on the way out the door for a graduate school interview and noticed that one of the lymph nodes in her neck was swollen. She called her doctor right away; he suggested she was probably catching a cold, blamed communal living and told her to make an appointment if the swelling did not decrease. Roberts got caught up in the stress of midterms and didn’t follow up even when the swelling persisted.
One night during the home stretch of her senior year, Roberts crawled into bed only to realize that she was afraid to fall asleep.
“I didn’t know if I was going to wake up in excruciating pain or not,” Roberts recalls. “I started thinking about the possibility that this could be something a lot more serious than I thought it was.”
She remembers then telling herself, “Oh my God, Elena, don’t be so melodramatic!”
For the next three months, every time she had those thoughts she pushed them away and told herself not to be dramatic.
Roberts made the most of her last few months on The Bluff, and when graduation rolled around, she was ready. She was handed a diploma in the Chiles Center on Sunday, May 1, 2016 with her family and closest friends in attendance.
Shortly after graduation, Roberts received word that she had been admitted into Duke University School of Medicine’s Master of Biomedical Sciences program.
Diploma in hand and Duke on the horizon, Roberts flew to Chicago to spend six weeks with O’Halloran while he finished up his graduate degree in International Security at the University of Chicago. She recalls only minimal pain during that time and had high hopes that “maybe it was getting better.”
She returned home to Medford, intending to only stay for a few weeks before her departure to Duke, where she would begin her path to becoming an emergency physician. She planned to spend time with family and tie up loose ends before starting her life’s next chapter.
But those few weeks turned into a year when she was forced to put her dreams on hold and fight cancer.
“You think you’re so healthy,” Roberts says, “and then to hear that you have a major afflicting disease… I was scared that everything I had worked so hard for was going to change.”
“Gap Year”
Roberts was diagnosed on June 29, the day before she was to fly to North Carolina and move into her apartment in Durham.
After breaking the news to her loved ones, her next call was to the airline to cancel her flight. And after that, to the guy who was supposed to deliver her newly-purchased but now unneeded bed. After that, apologetic messages to the two women she had planned to rent an apartment with, one of whom was vacationing in Iceland at the time. She remembers receiving only gracious responses.
All that was left was to call Duke.
She dialed and waited as she was passed through levels of the administration, as no one was quite sure how to handle a deferral in what was then only a two-year-old program. When she finally got on the phone with the Assistant Dean of Premedical Education Dr. Kathryn Adolsek, Adolsek assured her that Duke would wait for her.
“You don’t need to worry about Duke,” Adolsek told Roberts. “You have a spot here for as long as you would like it.”
According to the Leukemia and Lymphoma Society, there are five types of Hodgkin's Lymphoma cancer and Roberts’ type, Nodular Sclerosing, is the most common and most treatable, typically occurring in young adults between the ages of 15 and 34.
The cancer sets in when a white blood cell morphs into a lymphocyte cell, and the growing together of these lymphocytes forms clumps and masses, typically in the lymph nodes. The lower back and abdominal pain that Roberts suffered prior to her diagnosis was caused by the swelling of her lymph nodes.
O’Halloran flew from Houston to Medford two days after Roberts’ diagnosis, and stayed with her the rest of the summer as she went through the beginning of her treatment.
The two had been in a relationship for over a year.
“(I knew that) cancer was nothing compared to her strength and self determination,” O’Halloran said, though he was shocked and concerned for Roberts’ health.
Following her initial diagnosis, Roberts underwent a week-long outpatient staging process. It included five invasive procedures that would ultimately unveil the exact diagnosis and stage of her cancer.
The tests showed that the cancer in Roberts’ body was about to spread to her liver. Once the cancer has spread into at least one organ, it is considered Stage 4. Hodgkins Lymphoma is at its worst at Stage 4, at which point it has a 5-year survival rate of about 65 percent, according to the American Cancer Society. But since they caught it just in time, doctors confirmed that Roberts had Stage 3 cancer. At Stage 3, Roberts had an 80 percent chance of survival over five years.
They then tested her lung and heart function in preparation for chemotherapy.
“One of my chemo drugs can cause damage to the lungs and electrical functioning of the heart,” Roberts explained. “So they needed a baseline to use for comparison later in my treatment to determine if my chemo drugs were doing more harm than good.”
A small port was surgically implanted just below her collarbone on the right side of her chest. It was through this tube that her chemo would be administered for the next six months. Following the completion of her chemotherapy, Roberts would undergo another procedure to have the port removed.
Roberts’ first chemotherapy treatment took place Aug. 4, 2016.
Despite being a premed student, she knew little about the chemotherapy process.
“I knew that I would lose my hair,” she says, “and I would probably be really nauseous and I wouldn't really be able to eat any food and it would probably be a really miserable experience. I wasn’t looking forward to that.”

It turned out the only foods she couldn’t eat were cheese and sushi — two of her favorite things. Roberts later found out that this is due to the mold in cheese and the raw fish in sushi, and the vulnerable state that chemo would leave her body and immune system in.
She did not experience the nausea she expected, and says that food only tasted metallic for about three days after each treatment.
Roberts did lose her hair, but much later in the process than she anticipated.
“I really didn’t start losing hair significantly until November,” Roberts said, laughing. “Until then, I could still go out in public but would just fill in bald spots with eye shadow!”
In late November, Roberts asked her Godmother Melanie Breidenthal to shave her head.
The two women laughed together in the bathroom while Breidenthal shaved Roberts’ head, an experience unlike Roberts remembers seeing in movies when the scene is accompanied by crying and a feeling of defeat.
Breidenthal remembers the laughing and the bald jokes as well, but recalls having a different feeling inside.
“I felt so sad having to cut her hair, it’s so personal,” Breidenthal said. “But at the same time, I felt so honored to be the one who was doing it.”
Roberts, whose hair has yet to grow back, says she is OK with wearing wigs now because they keep her head warm during the winter and because her godsister, Geneva, 13, enjoys styling them.

O’Halloran watched as Roberts shifted from someone who had prioritized her beauty routine to someone who started to see that she was beautiful without it.
“Everytime I tell her that she’s beautiful, it’s like she finally started hearing it,” O’Halloran said.
Roberts says chemo was not as bad as she expected, despite side effects like memory loss, headaches, inconsistent energy and fatigue.
Roberts went into the clinic for one chemo treatment every two weeks. After her first four treatments, oncologists at her clinic in Medford, showed her two images of her full body scans. The first, taken before treatment began, shows the cancer lit up, and the second, only eight weeks into her treatment, shows no noticeable signs of cancer in her body. Despite this, it was still necessary for Roberts to undergo all 12 chemo treatments.
During her freshman year at UP, Roberts suffered from anxiety and depression. When she was able to work through those issues, she refocused her energy into health and fitness.
“I was really in shock because I had been healthy my whole life,” Roberts recalls about receiving her diagnosis, “Especially after the last couple years when I had really been committed to a fit and healthy lifestyle and I had been feeling better than I ever had in my life!”
Roberts, who is already a certified emergency medical technician (EMT) and aspires to be an emergency physician, had never so much as broken a bone.
Preparing for Grad School - Take Two
Six months removed from her diagnosis, Roberts now sees her overall experience as positive, but admits that this attitude did not come easily every day throughout her six months of treatment.
During moments when Roberts felt particularly low, she says she was inspired to continue her fight by Lindsey Walker, a fellow Medford resident who fought a long battle with cancer and ran a Facebook blog about it entitled “Lindsey’s Journey”. Walker found out her cancer was terminal in the fall and passed away on Dec. 18.
Roberts had not planned to spend this year in her hometown, but was welcomed in with open arms by her godmother Breidenthal’s family, whom Roberts considers her own. Both Roberts and Breidenthal are grateful for the opportunity, though under non-ideal circumstances, to spend time as a family this year. Roberts especially relishes in the time spent with Breidenthal’s children, Geneva, 13, and Austin, 5.
Austin, who does not yet have a real understanding of cancer, still gives Roberts gentle hugs “because she has cancer,” and is freaked out by her bald head.
Throughout Roberts’ treatment period, she has spent most of her days with Geneva and Austin, knitting, and craving cheese and sushi. Despite having symptoms that make it challenging, she still works hard to study for the Medical College Admission Test (MCAT).
Roberts had her last chemotherapy treatment on Jan. 12. She is officially cancer-free and in remission.
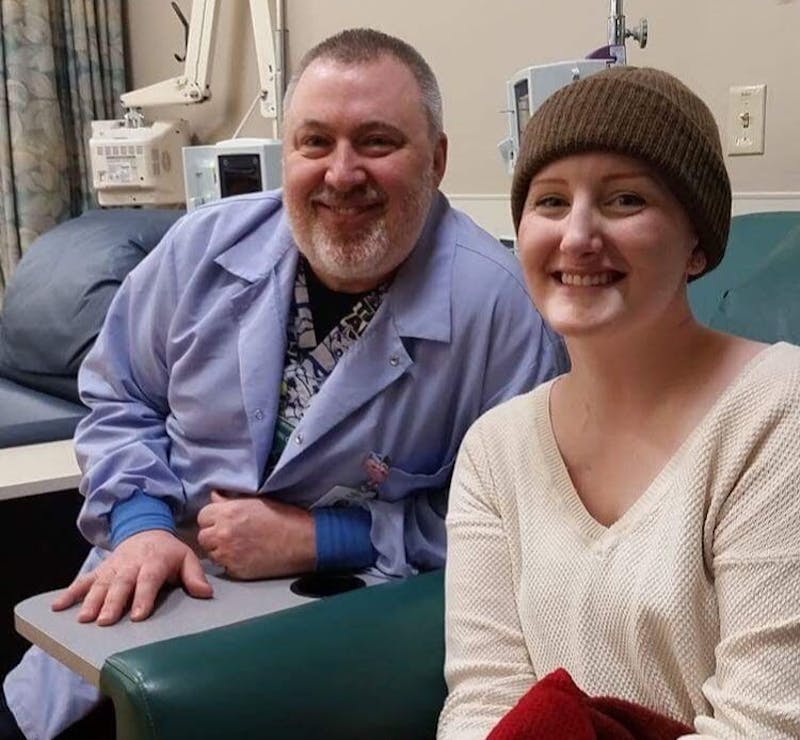
She is already planning a cheese party for which she envisions all-you-can-eat fondue, grilled cheese, mac n’ cheese and quesadillas.
Aside from the imminent cheese party, Roberts says her next few months will be spent studying for the MCAT, getting back into a workout routine and savoring the last few months with her family. She plans to take the MCAT in May, and will leave for Duke at the end of June, only one year behind schedule.
Her MCAT score will not affect her admission to Duke, but will be relevant to her medical school applications after she completes her 11-month masters program in Biomedical Sciences. Right now she is unsure of whether she will pursue a Medical Doctorate (M.D.) or a Doctorate of Osteopathic Medicine (D.O.).
Roberts has kept in contact with the Dean Andolsek from Duke with whom she corresponded after her initial diagnosis.
She recalls a recent letter from the Dean saying, “Our decision to defer you was an easy one. Good things are worth waiting for.” Roberts says she is grateful for their support.
Roberts, now cancer-free, is passionate about encouraging other young people to advocate for their own health.
“I was so committed to attaining a high GPA, applying to grad school, fulfilling my duties as an employee of KDUP, balancing all of my extracurricular activities, research, and volunteer work, maintaining a fit lifestyle, and being a present friend, girlfriend and family member, that I ignored very real concerns about my own health,” Roberts said. “I think I believed that prioritizing all of these commitments above a few stomach aches would somehow demonstrate my resiliency as a person.”
Former Oncology Social Worker Linda Cail reiterates this point when she says that many young people think that because they may be young, healthy or fit, that they are indestructible. Unfortunately, that is not always the case.
Each year in the United States, 60,000 young people between the ages of 20-39 are given a new cancer diagnosis, according to the American Cancer Society. While this is a relatively low number, Roberts wants to encourage other busy college students not to make her same mistake. Her symptoms ended up being obvious signs of a very serious illness that, if she would have caught at an earlier stage, may not have prevented her from going to Duke on schedule.
“No one else can experience your symptoms for you,” Roberts says. “No one but you can determine if what you are experiencing is having a noticeable impact on your daily life.”
Cail echoes this statement, encouraging young people to stay in tune with their bodies.
It is important to Roberts that her fellow Pilots know: “Your health, both physical and mental, always takes priority.”